The Opportunity
Victoria University and Western Health selected Portable to design and develop a new osteoarthritis pain intervention program platform, to provide advice and early interventions to help waitlist patients in the western suburbs of Melbourne manage their pain and improve their general health.
Based on several factors, such as personal circumstances, socio-demographic influences and access to health care, osteoarthritis patients on the waitlist to date were not receiving the timely support and advice they needed to intervene or prevent the deterioration of their current condition, with wait times sometimes extending to 3 years.
It was understood that if they had the support earlier in their patient journey, while they were on the waitlist, their condition could have been controlled, managed or even improved.
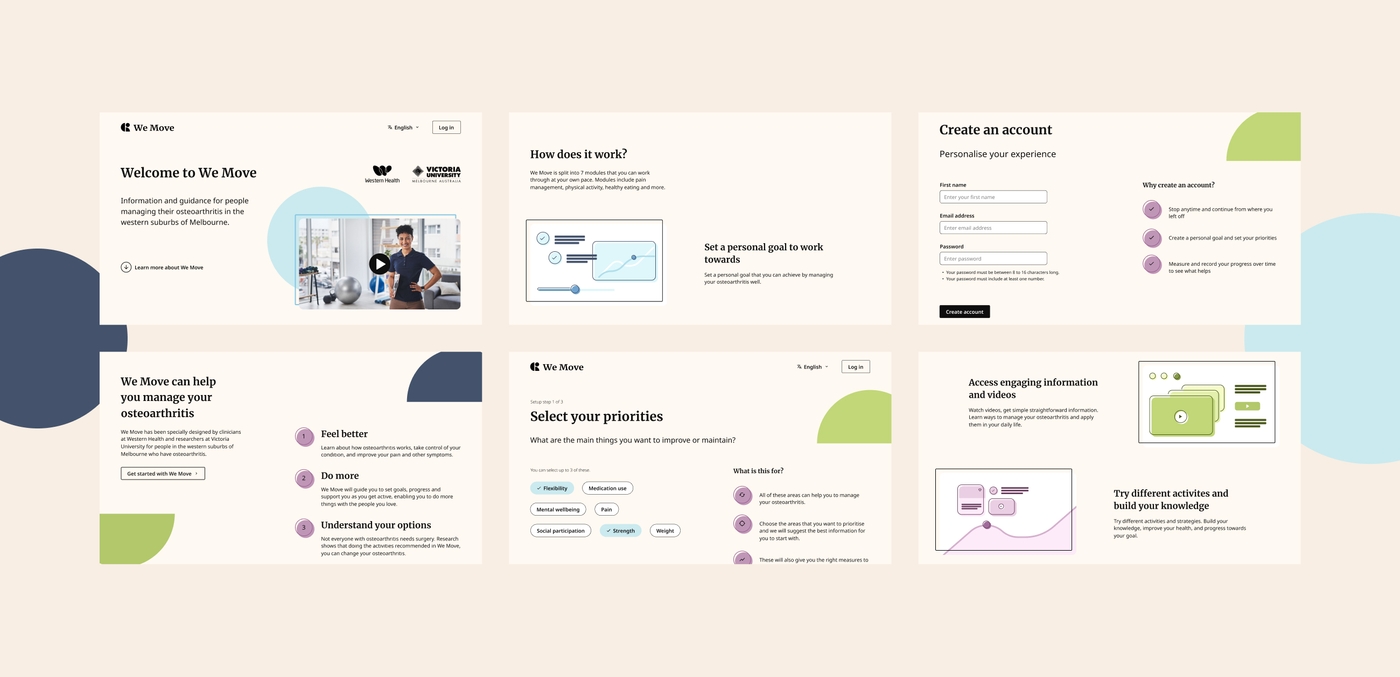
Victoria University and Western Health wanted the new platform to help patients to understand what holistic care is, what different possible lifestyle interventions there are, and how they can benefit people with osteoarthritis. Through Portable’s process of discovery, design and delivery, we were able to define the goals of the new digital platform, the “Why Wait” platform, and design a new MVP that provides osteoarthritis patients with health advice and guidance. Why Wait enables patients to:
- Engage with modular content on topics such as physical activity and diet
- The ability to set goals, track their progress through self-assessment and reflect on their achievements
- Access clear and accessible content providing practice solutions, activities and strategies for managing osteoarthritis.
The Challenge
The health and well-being of people living with osteoarthritis can deteriorate without any form of intervention, whether that’s surgical or nonsurgical. Meanwhile, wait times for osteoarthritis and joint replacement surgeries can stretch out for years.
Helping people with osteoarthritis to take early and independent intervention in regard to their condition can improve their health, reduce their rate of deterioration, improve their recovery from surgery – and even prevent the need for surgery altogether.
The challenge Victoria University and Western Health faced was complex and multi-faceted. By working with them early on we defined a design challenge to direct the engagement:
How might we design an online osteoarthritis intervention platform for people on a waitlist to see a specialist that is accessible, regardless of their health literacy or cultural and linguistic background, so that people can independently learn about their condition, seek accurate clinical advice and take tangible steps to improve their quality of life and potential surgery outcomes?
Our Approach
Kick-off workshops and client collaboration
We began with kick-off workshops to align the diverse project team from Victoria University, Western Health and Portable on the project aims and approach. We also worked together to define our research activities.
We decided that our priority was to first understand what challenges people with osteoarthritis currently face when trying to manage their condition, in order to get a sense of what an online intervention program would need to look like and include in order to be successful.
Discovery
The discovery phase included a series of 1:1 and group interviews with a range of clinicians, health professionals and providers. This gave us an insight into the different perspectives of different Osteo health professions such as surgeons and physiotherapists, the different touch points that people interact with on their health journeys and the challenges that both patients and clinicians face in managing or treating osteoarthritis.
Understanding the patient journey
From this we were able to map the current patient journey, their pain points and challenges and use this to start to uncover what an effective program might look like using real-world expertise, programs and approaches.
Establishing a strong design foundation
The project team used this journey map as a foundation for the design phase of the project. We translated all the insights, pain points and real-world experiences into actionable “How Might We” statements. We were then able to prioritise these statements into three categories:
- Fundamental problems to solve that will inform the core shape and function of the intervention program
- Impact drivers that will improve the use and efficacy of the solution we would design
- Future state problems that were beyond the scope of the project, but still impact to consider as part of our iterative design approach
Ideation
Once we had these statements and agreed on the categories, we embarked on an ideation process with Victoria University and Western Health. During these sessions, we came up with broad ideas for the intervention program, built on each other’s thinking and challenged our proposed solutions using real-world constraints. This approach helped us to define:
- The core content and design principles of the intervention program
- A comprehensive list of possible technical features and content topics
- An agreed core concept and design direction to begin wireframing and testing
Wireframing, prototyping and iterative design
Our Experience Design team got to work designing key pages and points of interaction for the online intervention program. First, we created low-fidelity wireframes and tested these people living with osteoarthritis in the western suburbs of Melbourne. These wireframes focused on cementing the functional aspects of the user experience and preferred content types of the people using the program.
With each version of the iterative design, the project team progressed from flat wire-framing to high fidelity and clickable prototypes; making sure to incorporate the latest testing insights and learnings. The wider Western Health and Victoria University teams were also kept in the loop with weekly showcases of the iterative designs.
Content collaboration with clinicians
Throughout the design process our Content Strategist collaborated closely with both Victoria University and Western Health. Using the insights uncovered from earlier research activities, we worked together to understand the content needs of people living with osteoarthritis so that they could feel comfortable and confident managing their condition independently.
The content strategist then worked alongside the Experience Designer team to establish a content structure for the overall intervention program and the individual subject modules within the program. This structure was included in the iterative user testing and any content-related insights learned were incorporated in future iterations.
Once we were confident in the program’s content approach, we provided the Victoria University and Western Health teams with a series of templates and writing and content guides so that they could independently produce the content needed for each module within the intervention program. Both the templates and guides took into consideration all the insights uncovered during the research phase plus healthcare content best practices – particularly for people with low health literacy or English as a second language.
Engaging with the local Vietnamese community
It was identified early in the project that we needed to ensure whatever we designed would help the diverse communities of the western suburbs. For the pilot version of the program, the Vietnamese community was selected as they are the largest culturally and linguistically diverse community in the western suburbs.
We worked with our partners, LOTE, to understand the Vietnamese community's patient journey, and who they want to receive their information from. It was identified through the project the Orthopaedic Surgeons' presence throughout the modules speaking both English and Vietnamese is paramount for the success of the program with the Vietnamese community.
Feature prioritisation
Throughout the project we worked closely with our technology team to make sure that the research-driven design and content approach also worked from a development point of view. We worked with both the project team and Victoria University and Western Health teams to prioritise the program’s features and decide what was essential for the program’s initial launch and what could be developed over time for future releases.
The features and requirements prioritised for the first release included:
- Personalised, pain intervention and health and lifestyle advice to people with osteoarthritis on the waitlist
- Compatible with desktop and mobile devices
- 8 weeks’ of modular content providing advice on lifestyle changes such as diet, mental wellbeing and exercise
- Accessible, visually pleasing and engaging for the primary audience of older people from Culturally and Linguistically Diverse (CALD) communities and clinicians
- Built-in analytics, to enable Victoria University to access and measure the program’s usage and enjoyment metrics
- Scalable component approach to provide an opportunity for multilingual accessibility and feature enhancements in the future
Technical stack
Based on the prioritised features, the technical stack chosen for this engagement was:
- We used Portable’s UI Toolkit to bootstrap the project with the latest integrations with Figma (our design tool of choice)
- Using the latest technologies from frameworks React, Next JS and Chakra UI
- Strapi CMS for all content management as well as user roles and security
Digital development
Once everything was agreed, our technology team set to work on:
- Building out a component library and design system for the chosen content management system (CMS), Strapi, which we selected as it has rich features for users, developers and ebay integration with front end frameworks and authentication
- Setting up a scalable cloud infrastructure, including enabling automated testing and future deployment pipelines
- Establishing a CMS design and content model so that the Victoria University content team could expand the program while maintaining a consistent user experience
- Creating user profiles and self-assessments components that enabled users to log in to their profile to continue their self-management and regularly assess their own progress
Project Outcomes
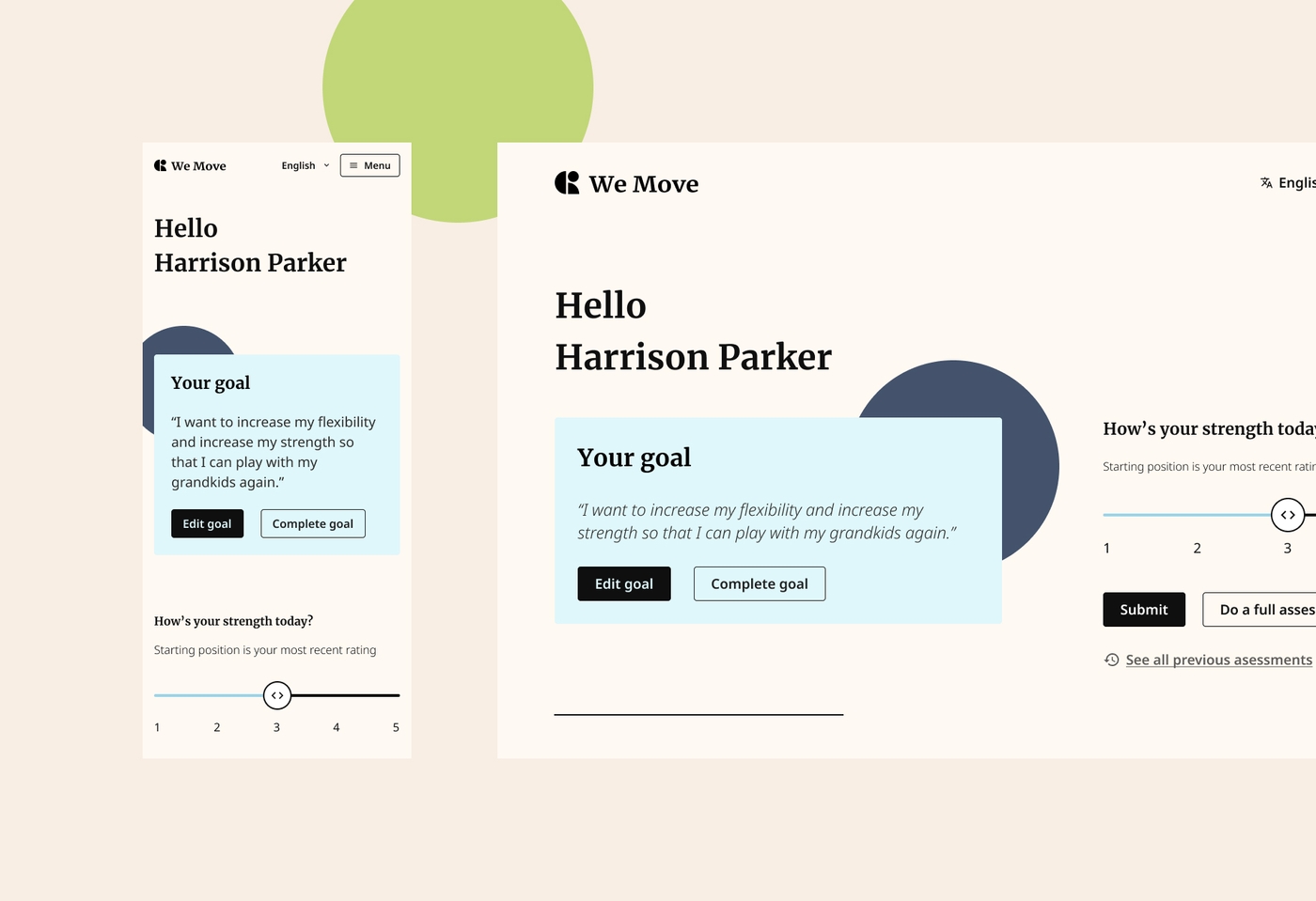
The key outcome of this project was a co-designed purpose-built online intervention program for people living with osteoarthritis in the western suburbs of Melbourne.
The online program enables users to create a secure account, set up personal health goals and track their progress, work through different modules on health and wellbeing – such as diet, mental health and exercise – and complete physical or interactive activities.
Thanks to a close partnership with multicultural marketing agency LOTE, the online intervention program also supports a completely integrated Vietnamese version of the program that users can seamlessly switch between. Enabling Vietnamese people living with osteoarthritis to fully benefit and participate in using this program to manage their osteoarthritis.
The iterative design approach we took means that the final structure of the online intervention program has flexibility embedded within it, enabling Western Health and Victoria University to expand the program to other osteo conditions in the future.
Emily Pearce, Senior Content Strategist:
“This project posed an interesting content challenge, to create an easy-to-follow intervention program to empower people with osteoarthritis to manage their condition independently – while also ensuring the content supported those with low health literacy and could be easily translated for the Vietnamese community of the Western suburbs.”
Project Team
- Tom Morris, Senior Digital Producer
- Ashlee West, Lead Experience Designer
- Dan Hoult, Senior Experience Designer
- Matt Dalla Rosa, Senior UX Researcher
- Emily Pearce, Senior Content Strategist
- Lincoln Le, Senior Developer
- Sonia Montero, Developer
- Prutha Kothari, Developer
- Andrew Fulton, Lead Developer